| Table of Contents |  |
|
Case Report
| ||||||
| A rare case of sigmoid perforation following argon laser coagulation of gastrointestinal amyloidosis | ||||||
| Animesh A. Singla1, Apresh A. Singla2 | ||||||
|
1MBBS, Senior Resident, Department of Surgery, Royal Prince Alfred Hospital, Sydney, NSW, Australia.
2MBBS, Registrar, Department of Surgery, Bankstown Hospital, Sydney, NSW, Australia. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article: |
| Singla A, Singla AA. A rare case of sigmoid perforation following argon laser coagulation of gastrointestinal amyloidosis. Edorium J Gastroenterol 2015;2:4–6. |
|
Abstract
|
|
Introduction:
Argon plasma coagulation (APC) is a safe technique to achieve endoscopic hemostasis and/or tissue ablation. Perforation is a rare complication. Gastrointestinal amyloidosis results in abnormal fibrillar protein deposition within the muscularis propria, leading to potential compromise in gut wall integrity.
Case Report: We report a rare case of iatrogenic sigmoid perforation secondary to APC treatment in a patient with recently diagnosed gastrointestinal amyloidosis. The patient initially presented with rectal (PR) bleeding with known gastrointestinal amyloidosis, and was found to have a lesion in her sigmoid colon. Hemostasis was achieved with APC therapy of the lesion. Over the next 24 hours, patient developed acute left iliac fossa tenderness with CT confirmed evidence of perforation. Urgent laparotomy was performed requiring rectosigmoidectomy with end colostomy. Conclusion: These patients may represent a high-risk group for APC treatment and may require additional precautions including limiting the time and intensity of treatment. | |
|
Keywords:
Amyloidosis, Argon plasma, Perforation
| |
|
Introduction
|
|
Argon plasma coagulation (APC) has been shown in vitro and in vivo to be a safe technique for endoscopic hemostasis and/or tissue ablation [1]. Colonic perforation is a rare complication, estimated at rate of approximately 0.27% in one study [2] . There have only been a handful of case reports where APC treatment of bleeding colonic polyps or angiodysplasia has resulted in perforation, necessitating acute surgical intervention [1] [3] [4] [5]. Gastrointestinal amyloidosis is a recognized entity that can cause per rectal (PR) bleeding [6]. This is more common is secondary amyloidosis, where abnormal extracellular protein deposition in the muscularis propria contributes to mucosal erosion. It contributes to weakening of all layers of the intestinal wall due to destruction of normal architecture, thus increasing fragility of the lesion [7]. We present the first case in literature to our knowledge of intestinal perforation secondary to APC treatment of gastrointestinal amyloidosis. They may represent a population at higher risk of such complication and appropriate care needs to be taken peri-procedurally for these patients. If perforation is suspected, timely diagnosis and surgical intervention is important to prevent mortality. |
|
Case Report
|
|
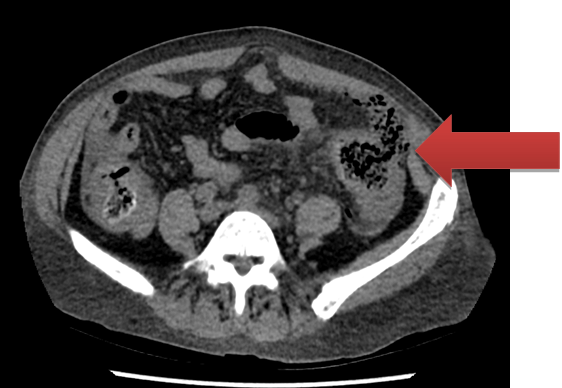
A 64-year-old female who presented to emergency room with fresh per rectal (PR) bleeding and clots. She had recently been diagnosed on biopsy with gastrointestinal amyloidosis, following a colonoscopy for a similar episode in the past. Her past medical history included multiple myeloma, which was treated successfully with stem cell transplantation. On this occasion, an urgent flexible sigmoidoscopy found a circumferential area of mucosal abnormality in the sigmoid colon consistent with active bleeding. She received argon plasma coagulation (APC) to the lesion with good hemostasis. Proximal to this, the colon appeared normal. Within the next 24 hours, the patient developed sudden onset of left lower quadrant pain with associated vomiting. The pain had no associated PR bleeding or diarrhea. On examination she was tachycardic, hypotensive but afebrile. She had tenderness and involuntary guarding in the left lower quadrant. An initial venous blood gas showed a pH 7.30, pCO2-61 and severe lactatemia. Computed tomography scan revealed a proximal sigmoid perforation with extensive intra-abdominal fecal material and pneumoperitoneum (Figure 1). The patient underwent an urgent laparotomy that identified a large 3 cm perforation in the sigmoid colon and extensive intra-peritoneal soiling. Patchy areas of subserosal/submucosal bruising were also noted in the cecum, descending colon and the remainder of sigmoid colon without any evidence of ischemia. She underwent a rectosigmoidectomy (Hartmann's) with end colostomy and subsequently was transferred to the ICU postoperatively. She made an uneventful recovery. Decision was made not perform a reversal of the colostomy due to the friable nature of remaining bowel. On sixth month follow-up the patient was progressing well with no complications. |
|
|
|
Discussion
|
|
We present a rare case of gastrointestinal perforation following argon plasma coagulation for an amyloidosis lesion. A previous case following APC treatment for gastrointestinal angiodysplasia reported epigastric pain clinically and CT evidence of pneumoperitoneum and submucosal emphysema. However, laparotomy failed to find an obvious perforation in a patient [8]. In another instance, a patient had undergone conservative management, with spontaneous resolution of the pneumoperitoneum [8]. It has recently been suggested that submucosal emphysema and pneumoperitoneum (due to the passage of air through the gut wall) following APC are more common than suspected and many remain asymptomatic [8] [9]. Lower gastrointestinal bleeding is the presenting symptom of colonic amyloidosis in 25–45% of cases, due to ulceration, ischemia or an infiltrative lesion [10]. Spontaneous perforation of gastrointestinal amyloidosis is uncommon but documented [7]. These patients are at risk as abnormal fibrillar protein deposition occurs in all layers of the intestinal lining and predisposes to weakening of the gastrointestinal wall [7]. As such, it is pertinent in these patients that CT evidence of free air and symptoms or signs of an acute abdomen should prompt an immediate laparotomy. In addition, due to this risk, extra precaution should be taken with APC in these patients. APC works by non-contact monopolar electrocautery using argon gas as the transport medium. Its advantage is that it has limited depth of injury as there is arcing of transmitted current away from treated area to non-treated areas with low resistance. This minimizes risk of perforation and thermal injury [1]. However, perforation due to thermal injury at the site of treatment can occur due to: violation of no-touch technique, high energy levels, extended application time and excessive gas flow rate [1] [11]. There is a paucity of case reports, but other documented complications include intestinal explosion due to inappropriate colon preparation, thermal burn of nearby staple line and stricture formation [1]. Further research is potentially warranted to assess APC treatment of bleeding lesions secondary to gastrointestinal amyloidosis. |
|
Conclusion
|
|
We present a case of gastrointestinal perforation secondary to APC treatment in a patient with known amyloidosis. Our case highlights that these patients are at a particularly increased risk and extra precautions may be required. These may include limiting the time and intensity of the treatment and having a low threshold for surgical intervention if patient demonstrates symptoms or signs of perforation. |
|
References
|
|
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions
Animesh A. Singla – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Apresh A. Singla – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Animesh A. Singla et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|